Bile Acid Diarrhoea
Written By Prem Nand, Clinical Dietitian - Nutritionist, NZRD Copyright: Maximised Nutrition 2025
Introduction
Bile Acid Diarrhoea (BAD) is an often-overlooked cause of chronic diarrhea. It occurs when bile acids, normally reabsorbed in the small intestine, enter the colon in excessive amounts. This leads to water and electrolyte secretion, increased colonic motility, and frequent, loose stools. Though commonly misdiagnosed as irritable bowel syndrome with diarrhoea (IBS-D), BAD affects up to one-third of IBS-D patients and around 1% of the general population (Walters & Pattni, 2010).
Understanding bile acid metabolism, its interaction with the gut microbiome, and the role of hepatic feedback regulation is essential to identifying and treating BAD effectively. This article explores the symptoms, causes, diagnostic tools, and treatment options for bile acid diarrhea.
What is Bile Acid Diarrhea
Bile acids (BAs) are synthesized from cholesterol in the liver and play a key role in fat digestion. After secretion into the small intestine, they emulsify dietary fats for absorption. Roughly 95% of these bile acids are reabsorbed in the terminal ileum and returned to the liver through the enterohepatic circulation (Hofmann, 2009a).
Amounts of Bile Acid Produced In Adult Humans
Graph below shows that the amounts that are typically produced in the adults (1).
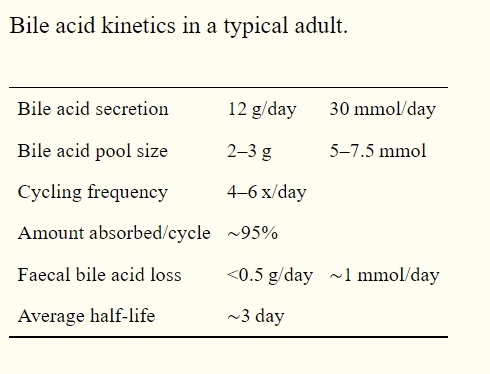
However, when this reabsorption process fails or bile acid production becomes excessive, too many bile acids reach the colon.
In the colon, bile acids stimulate secretion and increase motility, leading to diarrhoea, bloating, and gas. This condition—bile acid diarrhoea—was previously termed bile acid malabsorption (BAM), but newer evidence indicates that overproduction also plays a major role (Camilleri, 2020).
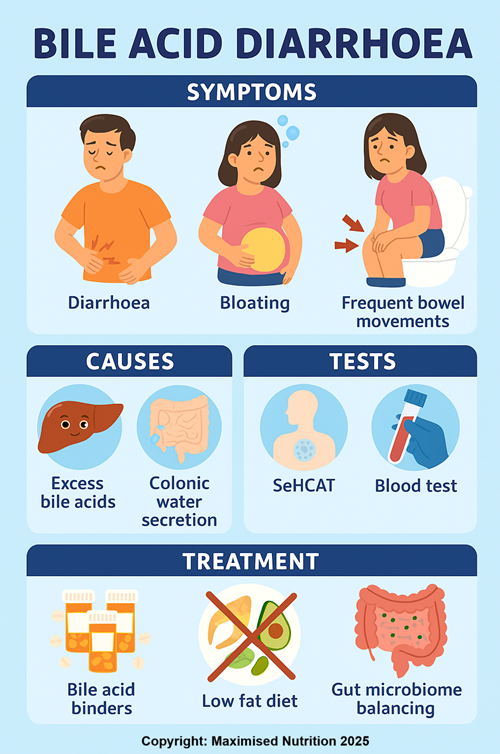
Symptoms of Bile Acid Diarrhoea
Patients with BAD typically experience:
• Chronic diarrhoea (often >5–6 bowel movements/day)
• Sudden urgency
• Bloating
• Flatulence
• Abdominal discomfort
These symptoms often mimic IBS-D, leading to underdiagnosis. However, unlike IBS-D, BAD is treatable with bile acid sequestrants and dietary changes.
Causes of Bile Acid Diarrhoea
There are three recognized types of bile acid diarrhoea:
Type 1: Ileal Disease or Resection
Damage to or removal of the terminal ileum, such as in Crohn’s disease or post-surgical resection, reduces bile acid reabsorption capacity, causing an overflow into the colon.
Type 2: Idiopathic BAD
This type occurs in people with no identifiable gut disease. Research suggests that a defect in the feedback loop involving fibroblast growth factor 19 (FGF19) leads to excessive hepatic bile acid synthesis (Walters et al., 2009).
Type 3: Secondary to Other Conditions
BAD may also occur as a result of:
• Cholecystectomy (gallbladder removal): Continuous bile acid release into the gut may overwhelm reabsorption.
• SIBO (Small Intestinal Bacterial Overgrowth): Disruption of bile acid metabolism by bacteria.
• Chronic pancreatitis or pancreatic enzyme insufficiency
• Coeliac disease or radiation enteritis
Each of these conditions disrupts normal bile acid regulation and increases the risk of diarrhoea.
Gut Microbiome and Bile Acid Transformation
The gut microbiota helps convert primary bile acids into secondary bile acids through microbial enzymes like bile salt hydrolase (BSH) and 7α-dehydroxylase. Species such as Clostridium scindens play an essential role in this process (Ridlon et al., 2014).
Disruptions in the microbiome—through antibiotic use, SIBO, or dysbiosis—may reduce these transformations, resulting in altered bile acid composition and increased diarrhoea (Shukla et al., 2014).
Diagnosis of Bile Acid Diarrhoea
SeHCAT Scan
The SeHCAT test involves swallowing a radiolabelled bile acid analogue and measuring retention after 7 days. A retention of less than 15% suggests BAD. Though highly effective, this test is not widely available in New Zealand.
Serum C4 (7α-hydroxy-4-cholesten-3-one)
This fasting blood test measures hepatic bile acid synthesis. Elevated levels (>48 ng/mL) suggest excessive bile acid production. While not commonly offered in New Zealand labs, it may be arranged via international reference laboratories (Camilleri, 2020).
FGF19 Blood Levels
Low fasting levels of FGF19 may indicate impaired bile acid feedback regulation, supporting a diagnosis of BAD.
Empirical Trial of Bile Acid Binders
In the absence of testing, many clinicians initiate a therapeutic trial of bile acid sequestrants. Symptom resolution can support the diagnosis.
Summary of Bile Acid Tests Available In New Zealand
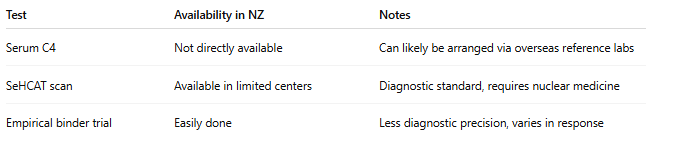
How Is BAD Different from IBS-D?
Many patients with chronic diarrhoea are misdiagnosed with IBS-D.
However, unlike IBS-D, bile acid diarrhoea has identifiable causes and responds well to specific treatments like bile acid sequestrants and low-fat diets. Identifying BAD can lead to significantly better quality of life (Wedlake et al., 2009).
Treatment Options for Bile Acid Diarrhoea
1. Bile Acid Sequestrants
These medications bind excess bile acids in the colon to prevent their diarrhoea-inducing effects:
• Cholestyramine: Effective but poorly tolerated due to texture and taste.
• Colesevelam: Better tolerated alternative.
• Colestipol: Less commonly used but may be effective.
Side effects include constipation, bloating, and interference with medication absorption.
Summary of Availability Of Bile Acid Medications In NZ
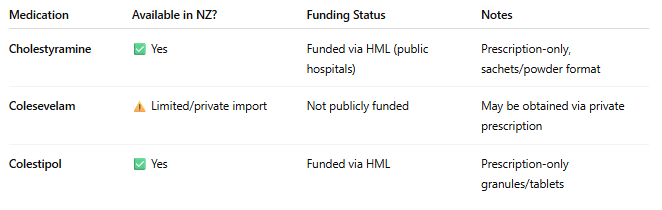
What Can You Do Next Regarding Medication?
Talk to your gastroenterologist or GP about which medication suits your case and availability.
Cholestyramine is widely available and funded—often first-line since it's accessible.
Colestipol may be used if bile acid sequestration is needed and hospital supply is appropriate.
Colesevelam is an effective and better-tolerated alternative—you’d likely need a private specialist prescription and to import it, which can involve additional costs and time.
2. Low-Fat Diet
Reducing dietary fat to <40g/day can help lower bile acid secretion, particularly beneficial in idiopathic or post-cholecystectomy cases (Wedlake et al., 2009).
3. Gut Microbiome Modulation
Probiotics and prebiotics targeting Clostridium species may help restore microbial bile acid metabolism and reduce diarrhoea. This area is still under investigation but holds promise (Shukla et al., 2014).
4. Treat Underlying Conditions
Addressing root causes such as SIBO, Crohn’s disease, or coeliac disease can help control BAD. Pancreatic enzyme supplementation may benefit those with chronic pancreatitis.
Prognosis and Quality of Life
When properly diagnosed and managed, bile acid diarrhoea is highly treatable. Many patients experience a rapid and significant improvement in bowel habits. However, undiagnosed BAD can lead to persistent discomfort, nutritional deficiencies, and reduced quality of life (Camilleri, 2020).
Key Takeaways

Conclusion
Bile Acid Diarrhoea is a common but under-recognized cause of chronic diarrhoea. It can result from malabsorption, hepatic overproduction, or altered microbiota. Diagnostic tools like the SeHCAT scan and serum C4 testing, though limited in availability, offer useful insights. Fortunately, BAD is highly manageable with targeted therapies, including bile acid binders and dietary changes. Increasing awareness among clinicians and patients is essential for better outcomes.
References
• Camilleri, M. (2020). Bile Acid diarrhea: prevalence, pathogenesis, and therapy. Gut and Liver, 14(5), 595–604. https://doi.org/10.5009/gnl19225
• Hofmann, A. F. (2009a). Bile acids: trying to understand their chemistry and biology with the hope of helping patients. Hepatology, 49(5), 1403–1418. https://doi.org/10.1002/hep.22789
• Keely, S. J., Walters, J. R., & Hore, T. A. (2020). Mechanisms of bile acid-induced diarrhoea. Nature Reviews Gastroenterology & Hepatology, 17(8), 445–457. https://doi.org/10.1038/s41575-020-0303-0
• Parry, S. A., Hodson, L., & Fielding, B. A. (2016). Bile acids and metabolic regulation in the liver, gut and adipose tissue. Digestive Diseases, 34(3), 337–344. https://doi.org/10.1159/000443860
• Ridlon, J. M., Kang, D. J., & Hylemon, P. B. (2014). Bile salt biotransformations by human intestinal bacteria. Journal of Lipid Research, 55(3), 396–411. https://doi.org/10.1194/jlr.R043513
• Shukla, P. K., Sunkara, R., & Sharma, N. (2014). Role of gut microbiota in bile acid metabolism and its clinical implications. Digestive Diseases and Sciences, 59(3), 409–416. https://doi.org/10.1007/s10620-013-2920-y
• Walters, J. R., & Pattni, S. S. (2010). Managing bile acid diarrhoea. Therapeutic Advances in Gastroenterology, 3(6), 349–357. https://doi.org/10.1177/1756283X10373846
• Walters, J. R., Tasleem, A. M., Omer, O. S., Brydon, W. G., Dew, T., & le Roux, C. W. (2009). A new mechanism for bile acid diarrhoea: defective feedback inhibition of bile acid biosynthesis. Clinical Gastroenterology and Hepatology, 7(11), 1189–1194. https://doi.org/10.1016/j.cgh.2009.06.023
• Wedlake, L., A’Hern, R., Russell, D., Thomas, K., & Andreyev, H. J. (2009). Systematic review: the prevalence of bile acid malabsorption as diagnosed by SeHCAT scanning in patients with diarrhoea-predominant irritable bowel syndrome. Alimentary Pharmacology & Therapeutics, 30(7), 707–717. https://doi.org/10.1111/j.1365-2036.2009.04092.x
• Wong, M. H., Rao, M. C., & Sellers, Z. M. (2012). Bile acids modulate tight junction structure and barrier function in the intestine. Laboratory Investigation, 92(4), 721–730. https://doi.org/10.1038/labinvest.2012.5
Quick Links
INFORMATION ON THIS WEBSITE IS FOR INFORMATIONAL PURPOSES ONLY.
PLEASE ALWAYS CONSULT A QUALIFIED HEALTH PRACTITIONER FOR A PERSONALISED ADVICE FOR YOUR HEALTH CONDITION
© 2025 MAXIMISED NUTRITION LTD. All Rights Reserved.



