Dangers of Misusing Nutritional Supplements
Author: Prem Nand, Clinical Dietitian - Nutritionist, NZRD Copyright Maximised Nutrition
Introduction
The inappropriate use of nutritional supplements is a growing public health concern. While supplements like vitamins, minerals, and herbal products are widely used to support wellness, using them incorrectly—without professional guidance—can lead to serious health risks. This article explores how inappropriate supplement use can harm the liver, kidneys, brain, and digestion, cause nutrient overload, and result in dangerous medication interactions. Read on for research-backed insights and practical safety guidelines.
What Is Inappropriate Supplement Use?
“Inappropriate use of nutritional supplements” refers to excessive, unsupervised, or misguided use of over-the-counter supplements. This includes:
• Taking supplements without a confirmed need
• Self-prescribing based on internet advice
• Exceeding safe dosages
• Ignoring drug-nutrient interactions
• Purchasing from unverified or unregulated sources
Despite being marketed as "natural," supplements are not automatically safe. In fact, they can cause organ damage, worsen chronic conditions, and interfere with medications if not taken properly (Mishra et al., 2022).
How Supplements Can Harm Major Organs

Liver: Risk of Hepatotoxicity
The liver metabolizes most supplements, making it especially vulnerable to toxic effects.
• Vitamin A toxicity may lead to liver fibrosis or failure when taken in excess (Penniston & Tanumihardjo, 2006).
• Green tea extract, kava, and black cohosh have been linked to liver inflammation and acute liver injury (Teschke et al., 2013).
• High-dose niacin used for cholesterol can also cause hepatotoxicity (Chitturi & Farrell, 2001).
Kidneys: Toxic Build-Up and Overload
The kidneys excrete excess nutrients, and overload can lead to damage.
• Vitamin D overuse causes calcium build-up in the kidneys (Marcinowska-Suchowierska et al., 2018).
• Protein powders, creatine, and herbal diuretics may harm kidney function in people with pre-existing renal issues (Poortmans & Dellalieux, 2000).
• Vitamin C in excess may contribute to kidney stone formation (Melnick et al., 2018).
Digestive Tract: Gut Imbalance and GI Upset
• Iron supplements often cause nausea and constipation (Bayraktar et al., 2021).
• Magnesium and zinc in excess can disrupt the gut and cause diarrhea.
• Probiotics, when misused, may cause gas, bloating, or bacterial overgrowth (Bafeta et al., 2018).
Nervous System and Brain: Neurological Risks
• Vitamin B6 megadosing has been linked to sensory nerve damage (Kawada et al., 2019).
• Melatonin misuse can impair circadian rhythms (Andersen et al., 2016).
• St. John's Wort may cause serotonin syndrome when combined with antidepressants (Fugh-Berman, 2000).

Nutrient Overload: More Is Not Always Better
Over-supplementation can lead to nutrient toxicity. Below is a table of commonly overdosed nutrients:
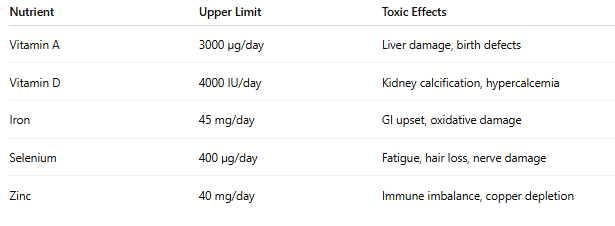
(Adapted from NIH Dietary Supplement Fact Sheets, 2022)
Nutrient interactions can also be problematic. For example, excess calcium reduces magnesium absorption and iron competes with zinc for uptake.
Drug–Supplement Interactions: Hidden Dangers
Common Interactions
Many people take supplements alongside prescribed medication, unaware of dangerous interactions:
• St. John’s Wort lowers the effectiveness of antidepressants and birth control pills (Izzo & Ernst, 2009).
• Vitamin K counteracts blood thinners like warfarin (Holbrook et al., 2005).
• Calcium and magnesium impair absorption of antibiotics like ciprofloxacin.
One study found that 20% of older adults take supplements that interact with their medications (Qato et al., 2018).
Herbal Interactions
Herbal products are especially risky because of unknown dosages and interactions.
• Ginkgo biloba increases bleeding risk.
• Ashwagandha may raise thyroid hormone levels (Choudhary et al., 2017).
• Ginseng affects blood sugar and can interfere with insulin or metformin.
Supplement Contamination and Poor Quality
Low-quality supplements may contain:
• Heavy metals like lead or mercury (Saper et al., 2008)
• Undeclared pharmaceuticals in weight loss or muscle-building products (Cohen et al., 2014)
• Synthetic fillers or allergens not disclosed on the label
Always look for third-party tested brands with GMP (Good Manufacturing Practice) certification.
At-Risk Populations
Certain groups should be extra cautious with supplement use:

Checklist: How to Take Supplement
Use this tick list before taking any supplement:
☑ Do I have a diagnosed deficiency or clinical need?
☑ Have I consulted a qualified health practitioner (nutritionist, naturopath, dietitian)?
☑ Is the brand certified for purity and safety?
☑ Am I taking the correct dose and form (e.g., methylated vs. standard B12)?
☑ Have I checked for interactions with medications or other supplements?
☑ Am I monitoring symptoms or lab values during use?
☑ Do I know how long to take this supplement?
☑ Have I considered getting nutrients through food first?
Conclusion: See a Qualified Practitioner Before Supplementing
Nutritional supplements are not harmless wellness tools—they are bioactive compounds that impact every system in the body. When misused, they can contribute to liver or kidney damage, nerve issues, digestive distress, and serious drug interactions.
⚠️ Always consult with a Clinical Dietitian - Nutritionist, or naturopath before starting any supplement. Personalized guidance can help you avoid harm and maximize your health outcomes.
Wondering how certain supplements affect gut health? Check out our guide on hydrogen methane breath testing
Discover how nutrition plays a vital role in managing complex conditions in our post on nutrition for rare disease.
References
Andersen, L. P. H., Gögenur, I., Rosenberg, J., & Reiter, R. J. (2016). The safety of melatonin in humans. Clinical Drug Investigation, 36(3), 169–175.
Bafeta, A., Koh, M., Riveros, C., Ravaud, P., & Ioannidis, J. P. A. (2018). Harms reporting in randomized controlled trials of interventions aimed at modifying microbiota: A systematic review. Annals of Internal Medicine, 169(4), 240–247.
Bailey, R. L., Gahche, J. J., Miller, P. E., Thomas, P. R., & Dwyer, J. T. (2013). Why US adults use dietary supplements. JAMA Internal Medicine, 173(5), 355–361.
Bayraktar, E. Ç., Yalçın, M. S., & Demir, A. M. (2021). Adverse effects of oral iron supplementation. Therapeutic Advances in Drug Safety, 12, 20420986211020249.
Chitturi, S., & Farrell, G. C. (2001). Hepatotoxicity of herbal medicines. Journal of Gastroenterology and Hepatology, 16(2), 132–139.
Choudhary, D., Bhattacharyya, S., & Bose, S. (2017). Efficacy and safety of Ashwagandha root extract in improving memory and cognitive functions. Journal of Dietary Supplements, 14(6), 599–612.
Cohen, P. A., Maller, G., & DeSouza, C. (2014). Presence of banned drugs in dietary supplements following FDA recalls. JAMA, 312(16), 1691–1693.
DiNicolantonio, J. J., O’Keefe, J. H., & Wilson, W. (2018). Subclinical magnesium deficiency: A principal driver of cardiovascular disease and a public health crisis. Open Heart, 5(1), e000668.
Fugh-Berman, A. (2000). Herb–drug interactions. The Lancet, 355(9198), 134–138.
Holbrook, A. M., Pereira, J. A., Labiris, R., McDonald, H., Douketis, J. D., Crowther, M., & Wells, P. S. (2005). Systematic overview of warfarin and its drug and food interactions. Archives of Internal Medicine, 165(10), 1095–1106.
Izzo, A. A., & Ernst, E. (2009). Interactions between herbal medicines and prescribed drugs. Drugs, 69(13), 1777–1798.
Kawada, Y., Ikenaka, Y., & Hirakawa, K. (2019). Sensory neuropathy induced by long-term overdose of vitamin B6. BMJ Case Reports, 12(2), e227263.
Manson, J. E., Cook, N. R., Lee, I. M., Christen, W., Bassuk, S. S., Mora, S., ... & Buring, J. E. (2019). Marine n−3 fatty acids and prevention of cardiovascular disease and cancer. New England Journal of Medicine, 380(1), 23–32.
Marcinowska-Suchowierska, E., Kupisz-Urbańska, M., Łukaszkiewicz, J., & Płudowski, P. (2018). Vitamin D toxicity–A clinical perspective. Frontiers in Endocrinology, 9, 550.
Melnick, J., Santos, J., & Catalano, R. A. (2018). Nephrotoxicity of vitamin C. Kidney360, 1(1), 25–30.
Mishra, S., Stierman, B., Gahche, J. J., & Potischman, N. (2022). Dietary supplement use in the United States, 2017–2018. NCHS Data Brief, 399, 1–8.
Navarro, V. J., Khan, I., Björnsson, E., Seeff, L. B., Serrano, J., & Hoofnagle, J. H. (2017). Liver injury from herbal and dietary supplements. Hepatology, 65(1), 363–373.
Penniston, K. L., & Tanumihardjo, S. A. (2006). Vitamin A toxicity. American Journal of Clinical Nutrition, 83(2), 191–201.
Poortmans, J. R., & Dellalieux, O. (2000). Do regular high-protein diets have potential health risks on kidney function in athletes? International Journal of Sport Nutrition and Exercise Metabolism, 10(1), 28–38.
Qato, D. M., Wilder, J., Schumm, L. P., Gillet, V., & Alexander, G. C. (2018). Changes in prescription and over-the-counter medication and dietary supplement use among older adults in the United States. JAMA Internal Medicine, 176(4), 473–482.
Rosenbush, M., & Reidenberg, M. M. (2001). Licorice-induced hypokalemia. Journal of Clinical Pharmacology, 41(3), 254–258.
Saper, R. B., Phillips, R. S., Sehgal, A., Khouri, N., Davis, R. B., Paquin, J., ... & Eisenberg, D. M. (2008). Lead, mercury, and arsenic in US- and Indian-manufactured Ayurvedic medicines sold via the Internet. JAMA, 300(8), 915–923.
Teschke, R., Frenzel, C., Schulze, J., & Eickhoff, A. (2013). Herbal hepatotoxicity: challenges and pitfalls of causality assessment methods. World Journal of Gastroenterology, 19(19), 2864–2882.
Vincent, J. B. (2003). The potential value and toxicity of chromium picolinate as a nutritional supplement, weight loss agent, and muscle development agent. Sports Medicine, 33(3), 213–230.
Zmora, N., Suez, J., & Elinav, E. (2018). You are what you eat: diet, health and the gut microbiota. Nature Reviews Gastroenterology & Hepatology, 15(1), 35–56.
Quick Links
INFORMATION ON THIS WEBSITE IS FOR INFORMATIONAL PURPOSES ONLY.
PLEASE ALWAYS CONSULT A QUALIFIED HEALTH PRACTITIONER FOR A PERSONALISED ADVICE FOR YOUR HEALTH CONDITION
© 2025 MAXIMISED NUTRITION LTD. All Rights Reserved.



