GLP-1 WEIGHT LOSS DRUGS: Long-Term Risks
Author: Prem Nand, Clinical Dietitian - Nutritionist, NZRD Copyright: Maximised Nutrition 2025
What Are GLP-1 Weight Loss Drugs?
GLP-1 weight loss drugs like Ozempic, Wegovy, Saxenda, and Mounjaro are prescription medications originally designed to treat type 2 diabetes. They work by mimicking natural gut hormones that help control appetite and blood sugar.
These drugs are now widely used to support weight loss—even for people who don’t have diabetes. They can be effective, but they also come with long-term risks that are important to understand.
If you're using these medications or considering them, it's essential to combine them with the right nutrition and lifestyle habits to stay healthy and avoid serious side effects.

How Do GLP-1 Medications Work?
GLP-1 stands for glucagon-like peptide-1. It’s a hormone that:
• Helps the pancreas release insulin
• Reduces appetite by acting on the brain
• Slows how fast food leaves the stomach
Drugs like Semaglutide (Ozempic, Wegovy) and liraglutide (Saxenda) copy this hormone to help reduce hunger and support weight loss (Nauck & Meier, 2019).
Mounjaro (tirzepatide) is a newer drug that also mimics another hormone called GIP, making it even more effective for some people (Frías et al., 2021).
Benefits of GLP-1 Weight Loss Drugs
Clinical trials show impressive results from these medications:
• Wegovy users lost about 15% of their body weight over 68 weeks (Wilding et al., 2021)
• Mounjaro users lost up to 21% of their body weight in one trial (Jastreboff et al., 2022)
• Blood sugar, cholesterol, and blood pressure also improved in many participants
These are real benefits—especially for people with obesity or metabolic health issues.
Taciti arcu porttitor a magna torquent risus diam, ultrices aliquam. Quisque tellus venenatis vitae fermentum molestie leo, elementum vehicula fringilla dolor magna quis, justo risus!
Long-Term Risks of GLP-1 Weight Loss Drugs
While GLP-1 drugs are powerful, they’re not risk-free. Here are some of the long-term concerns:
1. Digestive Issues
Common side effects include:
• Nausea
• Vomiting
• Constipation or diarrhoea
These can affect up to 80% of users, especially when starting or increasing the dose (Bhatti et al., 2023). In rare cases, the stomach slows down too much, leading to gastroparesis (Ghoshal et al., 2023).
2. Gallbladder Problems
GLP-1 drugs increase the risk of gallstones and gallbladder inflammation, especially during rapid weight loss (Faillie et al., 2016).
3. Pancreatitis
Some people have developed inflammation of the pancreas while taking these drugs. While rare, this side effect can be serious and needs immediate attention (Wang et al., 2022).
4. Thyroid Tumors
Animal studies found a link between GLP-1 drugs and thyroid tumors. The risk in humans is unclear, but the drugs are not recommended for people with a family history of thyroid cancer (Marso et al., 2016).
5. Muscle and Bone Loss
Rapid weight loss can lead to muscle and bone loss if you’re not eating enough protein or exercising regularly. One study found up to 39% of the lost weight was lean tissue (Lundgren et al., 2021).
6. Nutrient Deficiencies
Because these drugs reduce your appetite, you may end up eating too little, which can lead to low levels of:
• Vitamin B12
• Iron
• Calcium
• Vitamin D (Trujillo et al., 2021)
7. Hair and Skin Changes
Some people experience hair thinning or facial volume loss—known online as “Ozempic face” (Hajduch et al., 2023).
8. Mental Health Concerns
GLP-1 drugs affect brain chemistry. Some users report mood changes, anxiety, or low motivation. These effects are rare, but should be monitored (Müller et al., 2023).
What Happens When You Stop Taking GLP-1 Drugs? One of the biggest concerns is weight regain after stopping the medication.
In a follow-up to the Wegovy trial, participants regained about two-thirds of the weight they had lost within one year of stopping the drug (Wilding et al., 2022).
This shows that these medications don’t offer a “cure” for weight issues. They’re a tool—but they must be used as part of a long-term plan that includes nutrition, movement, and mindset.
Nutrition and Lifestyle Tips for Safe Use If you're taking GLP-1 medications, here are expert-backed tips to stay healthy and make your weight loss last:
1. Eat Enough Protein
To protect your muscle mass, aim for:
• 1.2 to 1.5 grams of protein per kg of body weight per day
• Include protein in every meal (chickpeas, tofu, lentils, eggs, fish)
(Hébuterne et al., 2022)
2. Do Strength Exercises
You don’t need a gym. Resistance bands or bodyweight moves help keep your muscles and bones strong. Aim for 2–3 sessions per week.
3. Watch for Nutrient Deficiencies
Ask your doctor or dietitian to check your levels of:
• Vitamin B12
• Iron
• Calcium and Vitamin D
Supplements may be needed, especially in people over 50 or those with limited diets.
4. Support Your Gut To reduce side effects like bloating and nausea:
• Eat smaller meals
• Stay hydrated
• Slowly increase fiber (e.g., oats, flaxseed)
• Include probiotics (e.g., sauerkraut, kefir, or supplements)
(Rosenbaum et al., 2021)
5. Look After Your Mental Health
Weight loss can affect emotions, self-esteem, and body image. If you're feeling overwhelmed, seek help from a:
• Psychologist
• Counsellor
• Dietitian with experience in emotional eating
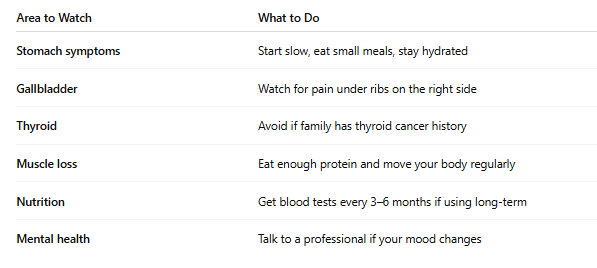
Use These Medications Safely
Final Thoughts
GLP-1 weight loss drugs like Ozempic, Wegovy, and Mounjaro can offer big benefits—but they also come with real risks, especially when used without support.
By focusing on nutrition, strength, hydration, emotional health, and regular check-ups, you can reduce those risks and build long-term success.
If you’re on one of these medications or thinking about it, talk to a health professional—especially a registered dietitian who is specialised in weight loss, gut health, hormonal health—to create a safe, supported plan for your weight and overall health.
Want More Support?
If you found this article helpful, share it with someone using a GLP-1 medication. For personalized advice, reach out to Prem Nand, Integrative Clinical Dietitian - Nutritionist, NZRD
References
Aronne, L. J., Wadden, T. A., Peterson, C., Gadde, K. M., Ryan, D. H., & Kushner, R. F. (2023). Managing the adverse effects of GLP-1 receptor agonists in obesity treatment. Obesity, 31(1), 9–16. https://doi.org/10.1002/oby.23698
Bhatti, A., Kalamegam, S., Shaikh, R., & Jameel, M. (2023). A review of the gastrointestinal side effects of GLP-1 receptor agonists. Cureus, 15(3), e35971. https://doi.org/10.7759/cureus.35971
Butler, P. C., Elashoff, M., Elashoff, R., & Gale, E. A. M. (2013). A critical analysis of the clinical use of incretin-based therapies: Are the GLP-1 therapies safe? Diabetes Care, 36(7), 2118–2125. https://doi.org/10.2337/dc12-2504
Drucker, D. J. (2018). Mechanisms of action and therapeutic application of glucagon-like peptide-1. Cell Metabolism, 27(4), 740–756. https://doi.org/10.1016/j.cmet.2018.03.001
Faillie, J. L., Yu, O. H., Yin, H., & Suissa, S. (2016). Association of incretin-based drugs with the risk of gallbladder disease. JAMA Internal Medicine, 176(5), 655–662. https://doi.org/10.1001/jamainternmed.2016.0441
Frías, J. P., Davies, M. J., Rosenstock, J., et al. (2021). Tirzepatide versus semaglutide once weekly in patients with type 2 diabetes. The New England Journal of Medicine, 385, 503–515. https://doi.org/10.1056/NEJMoa2107519
Gerstein, H. C., Colhoun, H. M., Dagenais, G. R., et al. (2019). Dulaglutide and cardiovascular outcomes in type 2 diabetes (REWIND): A double-blind, randomized placebo-controlled trial. The Lancet, 394(10193), 121–130. https://doi.org/10.1016/S0140-6736(19)31149-3
Ghoshal, U. C., Singh, R., Palit, A., & Srivastava, D. (2023). Gastroparesis in the era of incretin-based therapies. World Journal of Gastroenterology, 29(15), 2139–2152. https://doi.org/10.3748/wjg.v29.i15.2139
Hébuterne, X., Bermon, S., & Schneider, S. M. (2022). Preventing muscle loss in obesity management with GLP-1 RAs. Clinical Nutrition ESPEN, 48, 205–210. https://doi.org/10.1016/j.clnesp.2022.02.007
Jastreboff, A. M., Aronne, L. J., Ahmad, N. N., et al. (2022). Tirzepatide once weekly for the treatment of obesity. The New England Journal of Medicine, 387, 205–216. https://doi.org/10.1056/NEJMoa2206038
Lundgren, J. R., Batterham, R. L., Christensen, R. H., et al. (2021). Healthy weight loss without muscle loss: A challenge for obesity treatment. The Lancet Diabetes & Endocrinology, 9(11), 741–749. https://doi.org/10.1016/S2213-8587(21)00239-8
Marso, S. P., Daniels, G. H., Brown-Frandsen, K., et al. (2016). Liraglutide and cardiovascular outcomes in type 2 diabetes. The New England Journal of Medicine, 375(4), 311–322. https://doi.org/10.1056/NEJMoa1603827
Müller, T. D., Finan, B., Clemmensen, C., et al. (2023). The neuropsychiatric profile of GLP-1-based therapies. Nature Reviews Endocrinology, 19, 144–158. https://doi.org/10.1038/s41574-022-00783-4
Nauck, M. A., & Meier, J. J. (2019). Incretin hormones: Their role in health and disease. Diabetes, Obesity & Metabolism, 21(S1), 5–21. https://doi.org/10.1111/dom.13642
Rosenbaum, M., Yu, X., & Leibel, R. L. (2021). Gut microbiota and obesity: Interactions with GLP-1. Trends in Endocrinology & Metabolism, 32(7), 489–500. https://doi.org/10.1016/j.tem.2021.04.003
Trujillo, J. M., Nuffer, W., & Ellis, S. L. (2021). GLP-1 receptor agonists: An evidence-based review of safety and tolerability. Clinical Diabetes and Endocrinology, 7(1), 5. https://doi.org/10.1186/s40842-021-00117-z
Wilding, J. P. H., Batterham, R. L., Calanna, S., et al. (2021). Once-weekly semaglutide in adults with overweight or obesity. The New England Journal of Medicine, 384, 989–1002. https://doi.org/10.1056/NEJMoa2032183
Wilding, J. P. H., Bailey, C. J., & Kalra, S. (2022). Weight regain after semaglutide discontinuation: Implications for chronic obesity treatment. Obesity Reviews, 23(11), e13467. https://doi.org/10.1111/obr.13467
Wang, S., Sun, Y., & Liu, X. (2022). The risk of pancreatitis associated with GLP-1 receptor agonists: A meta-analysis. Diabetes Therapy, 13(6), 1355–1364. https://doi.org/10.1007/s13300-022-01240-z
Quick Links
INFORMATION ON THIS WEBSITE IS FOR INFORMATIONAL PURPOSES ONLY.
PLEASE ALWAYS CONSULT A QUALIFIED HEALTH PRACTITIONER FOR A PERSONALISED ADVICE FOR YOUR HEALTH CONDITION
© 2025 MAXIMISED NUTRITION LTD. All Rights Reserved.



