Is Chronic Inflammation Sneaking Up on You? Find out in just 60 seconds with this simple test

Hydrogen Methane Breath Test Explained: Which is better: Lactulose or Glucose?
Sub-heading
Author: Prem Nand, NZRD (Clinical Dietitian - Nutritionist) Published May 2026 Copyright: Maximised Nutrition Ltd
Introduction
Bloating after meals, excessive gas, constipation, diarrhoea, reflux, and brain fog are common symptoms experienced by people diagnosed with Irritable Bowel Syndrome. In many cases, these symptoms may be linked to an overgrowth of microbes in the small intestine rather than a problem with the bowel itself.
The hydrogen methane breath test is a non-invasive test that can help identify Small Intestinal Bacterial Overgrowth and Intestinal Methanogen Overgrowth. At Maximised Nutrition, I use lactulose as the preferred test substrate because it provides a more comprehensive assessment of the entire small intestine.
This article explains how the hydrogen-methane breath test works, the differences between lactulose and glucose, and why test results should always be interpreted in the context of a full clinical assessment.
What Is Hydrogen Methane Breath Test?
Hydrogen methane breath testing measures gases produced when microbes ferment carbohydrates in the digestive tract.
Humans do not produce hydrogen or methane on their own. These gases are generated by microorganisms in the gut:
• Certain bacteria produce hydrogen.
• Methane is primarily produced by methanogenic archaea, especially Methanobrevibacter smithii.
• Hydrogen sulfide is another important gas, although it is not routinely tested in New Zealand at present.
These gases are absorbed into the bloodstream, carried to the lungs, and then exhaled. By collecting breath samples over several hours, clinicians can identify abnormal fermentation patterns suggestive of microbial overgrowth (Rezaie et al., 2017).

What Conditions Can Hydrogen Methane Breath Test Detect?
Hydrogen methane breath testing may help identify:
• Small Intestinal Bacterial Overgrowth (SIBO)
• Intestinal Methanogen Overgrowth (IMO)
• Carbohydrate fermentation abnormalities
• Abnormal intestinal transit patterns
Small Intestinal Bacterial Overgrowth (SIBO)
SIBO occurs when excessive numbers of bacteria colonise the small intestine, where bacterial concentrations are normally much lower than in the colon.Intestinal Methanogen Overgrowth (IMO)
IMO refers to an overgrowth of methane-producing archaea. Methane is associated with slower intestinal transit and is strongly linked with constipation (Pimentel et al., 2006).
Symptoms That May Suggest SIBO or IMO
Common symptoms include:• Bloating
• Excessive gas
• Constipation
• Diarrhoea
• Alternating bowel habits
• Reflux
• Abdominal discomfort
• Brain fog
• Fatigue
• Food intolerances
• Iron, vitamin B12, or other nutrient deficiencies
These symptoms may overlap with IBS, but in some people they reflect an underlying microbial imbalance.
How Hydrogen Methane Breath Test Works
The test involves:
1. Following a special preparation diet.
2. Fasting overnight.
3. Providing a baseline breath sample.
4. Drinking a carbohydrate substrate (lactulose or glucose).
5. Collecting breath samples every 20 minutes for approximately three hours.
The pattern and timing of gas production are then interpreted alongside symptoms and clinical history.
Lactulose vs Glucose: What Is the Difference?
The two most commonly used substrates for SIBO breath testing are lactulose and glucose.
Glucose Breath Testing
Glucose is rapidly absorbed in the upper small intestine. If bacteria are present in the proximal small intestine, they ferment glucose before it is absorbed, resulting in measurable hydrogen and/or methane.Advantages of Glucose Testing
• Higher specificity in some studies
• Less likely to be influenced by colonic fermentation
• Useful when overgrowth is primarily proximal
Limitations of Glucose Testing
• May miss bacterial overgrowth in the middle or distal small intestine
• Limited ability to assess the entire small bowel
• Reduced sensitivity in some patients (Rezaie et al., 2017)
Because glucose is absorbed quickly, overgrowth located further downstream may not be exposed to enough substrate to generate a measurable response.
Lactulose Breath Testing
Lactulose is a non-absorbable synthetic sugar that passes through the entire small intestine before entering the colon.Advantages of Lactulose Testing
• Assesses the full length of the small intestine
• May better detect distal overgrowth
• Useful for methane-dominant constipation cases
• Provides information about intestinal transit patterns
Limitations of Lactulose Testing
• Interpretation requires experience
• Colonic fermentation can complicate analysis if timing is not considered carefully
Despite these challenges, lactulose provides a broader view of small bowel fermentation and motility.
Why I Prefer Lactulose in Clinical Practice
At Maximised Nutrition, I prefer lactulose because it allows assessment of the entire small intestine rather than only the upper section.This is particularly important for people with:
• Chronic constipation
• Methane-dominant patterns
• Slow gut motility
• Post-surgical anatomy
• Suspected distal small bowel overgrowth
During a professional webinar, one point that resonated strongly was that some patients presenting for breath testing may have been eating poorly or restricting food intake. In such situations, the degree to which glucose is absorbed before reaching more distal regions of the small intestine may reduce the likelihood of detecting overgrowth. While this concept has not been established as a formal guideline, it aligns with the practical limitation that glucose is rapidly absorbed and may not adequately challenge the entire small bowel.
For this reason, lactulose is my preferred substrate when the goal is to obtain a comprehensive assessment.
Sensitivity and Specificity of Breath Testing
No breath test is perfect. Accuracy varies depending on the substrate used and the reference standard.
Sensitivity and specificity are measures used to describe how well a diagnostic test performs.
Sensitivity refers to the ability of a test to correctly identify people who truly have the condition (the true positive rate). A highly sensitive test is less likely to miss cases, resulting in fewer false negatives.
Specificity refers to the ability of a test to correctly identify people who do not have the condition (the true negative rate). A highly specific test is less likely to incorrectly label healthy individuals as having the condition, resulting in fewer false positives.
In clinical practice, both measures are important because they help clinicians understand how reliable a test is and how much confidence can be placed in the results when interpreted alongside symptoms and medical history.
A systematic review reported approximate ranges as follows (Khoshini et al., 2008):
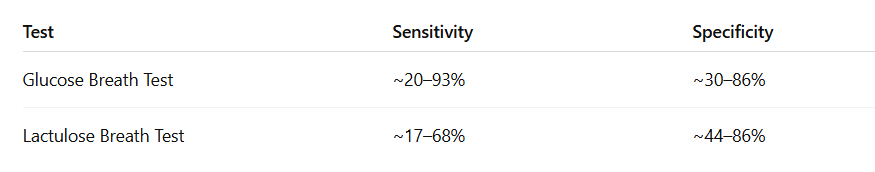
These wide ranges reflect differences in methodology and the limitations of small bowel aspirate culture as a reference standard.
What This Means Clinically
• A positive test should be interpreted in the context of symptoms and medical history.
• A negative test does not completely exclude microbial overgrowth.
• Clinical judgment remains essential.
Methane and Constipation
Methane has a direct slowing effect on intestinal transit. In experimental studies, methane exposure slowed bowel movement speed by approximately 59% (Pimentel et al., 2006).
Current North American consensus guidelines define a methane level of 10 parts per million (ppm) or higher at any time during the test as supportive of intestinal methanogen overgrowth (Rezaie et al., 2017).
This is one reason why hydrogen methane breath testing is especially useful in patients with chronic constipation.
Why I Do Not Routinely Use Lactose or Fructose Breath Tests
Although lactose and fructose breath tests are widely available, I do not routinely use them in practice.
Limitations Include
• Results may not correlate well with real-life symptoms.
• Positive tests can occur in individuals who tolerate the food well.
• Symptoms depend on dose, meal composition, gut microbiome, and transit time.
• False positives and false negatives are common.
My Preferred Approach
Rather than relying solely on lactose or fructose breath tests, I assess:
• Food tolerance history
• Portion sizes
• Symptom patterns
• Overall gut health
• Structured dietary trials
This approach often provides more clinically meaningful information and leads to practical recommendations.
What Happens After the Test?
Hydrogen methane breath testing is only one part of the assessment.
Following testing, results are integrated with:
• Medical history
• Medications
• Bowel patterns
• Nutrition intake
• Stress and lifestyle factors
A personalised plan may include:
• Dietary modification
• Motility support
• Targeted antimicrobial strategies
• Microbiome rehabilitation
• Correction of nutrient deficiencies
Hydrogen Methane Breath Testing in New Zealand
At Maximised Nutrition, I offer home-based hydrogen methane breath testing using lactulose, together with a comprehensive interpretation and personalised nutrition plan.
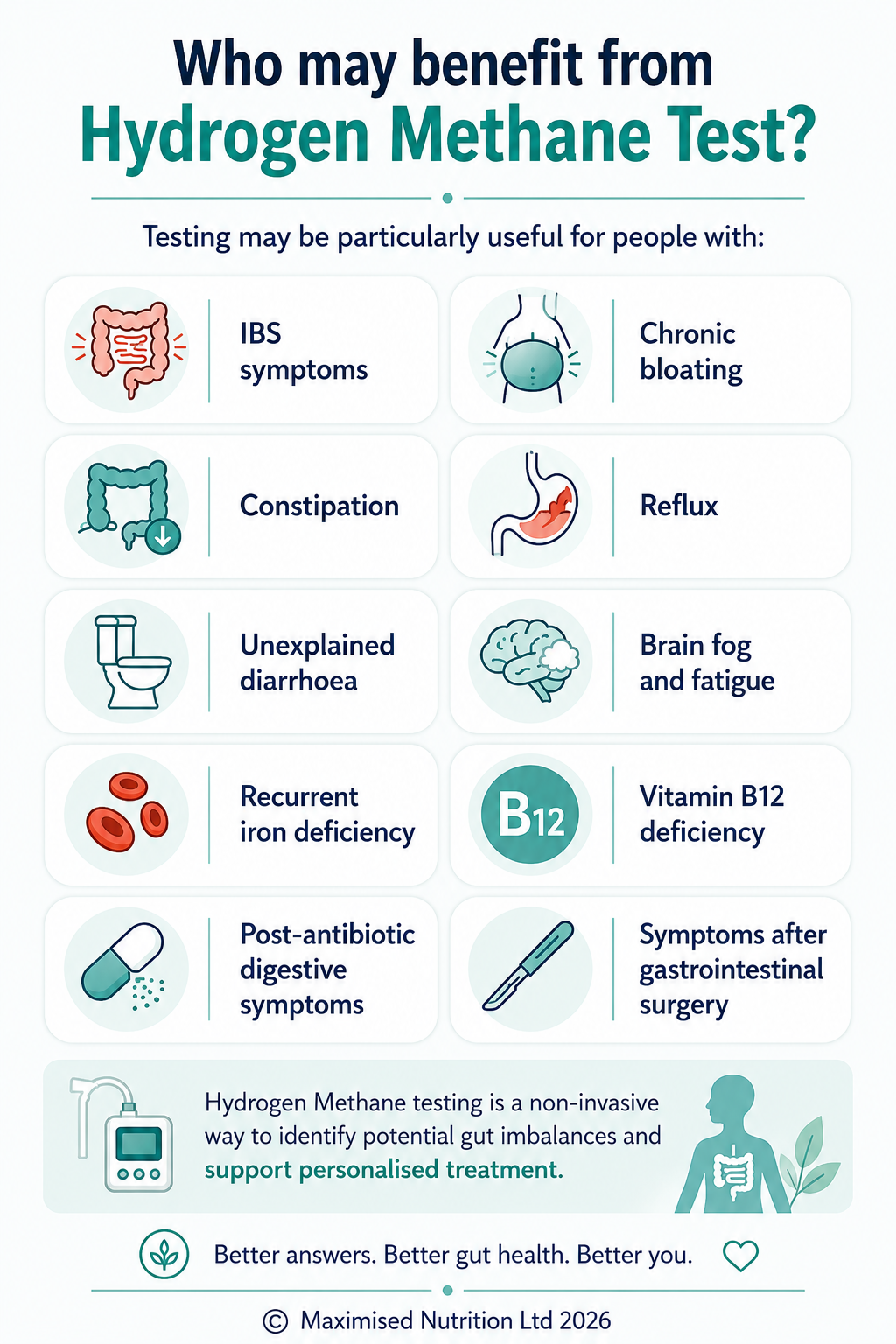
This service is particularly helpful for people experiencing:
• Chronic bloating
• IBS symptoms
• Constipation
• Reflux
• Food intolerances
• Unexplained digestive symptoms
Final Thoughts
Hydrogen methane breath testing is a valuable tool for identifying hidden microbial imbalances that may contribute to digestive symptoms.
Although both glucose and lactulose are accepted substrates, I prefer lactulose because it passes through the entire small intestine and provides a broader assessment of fermentation and motility.
When interpreted alongside a thorough clinical assessment, hydrogen methane breath testing can offer meaningful insights and help guide a more targeted and effective treatment plan.
Frequently Asked Questions
Is lactulose better than glucose for SIBO testing?
Lactulose is non-absorbable and assesses the full small intestine, while glucose is rapidly absorbed and may miss distal overgrowth.What does methane on a breath test mean?
Methane is associated with slower bowel motility and is commonly linked with constipation.Can a breath test explain bloating and constipation?
Yes. Hydrogen methane breath testing can identify microbial patterns that may contribute to these symptoms.Are lactose and fructose breath tests accurate?
Their clinical usefulness is limited because results do not always correlate with real-life tolerance.References
Khoshini, R., Dai, S. C., Lezcano, S., & Pimentel, M. (2008). A systematic review of diagnostic tests for small intestinal bacterial overgrowth. Digestive Diseases and Sciences, 53(6), 1443–1454.
Pimentel, M., Lin, H. C., Enayati, P., et al. (2006). Methane, a gas produced by enteric bacteria, slows intestinal transit and augments small intestinal contractile activity. American Journal of Physiology-Gastrointestinal and Liver Physiology, 290(6), G1089–G1095.
Pimentel, M., Saad, R. J., Rao, S. S. C., et al. (2020). ACG Clinical Guideline: Small intestinal bacterial overgrowth. American Journal of Gastroenterology, 115(2), 165–178.
Rezaie, A., Buresi, M., Lembo, A., et al. (2017). Hydrogen and methane-based breath testing in gastrointestinal disorders: The North American consensus. American Journal of Gastroenterology, 112(5), 775–784.

About the Author
Prem Nand, NZRD, is an Integrative Clinical Dietitian–Nutritionist and founder of Maximised Nutrition
in New Zealand. She uses a whole-body, systems-based nutrition approach to support people with complex and medically layered health conditions, considering the interconnected role of the gut, brain, nervous system, hormones, metabolism, inflammation, and lifestyle factors in human health.
Quick Links
INFORMATION ON THIS WEBSITE IS FOR INFORMATIONAL PURPOSES ONLY.
PLEASE ALWAYS CONSULT A QUALIFIED HEALTH PRACTITIONER FOR A PERSONALISED ADVICE FOR YOUR HEALTH CONDITION
© 2025 MAXIMISED NUTRITION LTD. All Rights Reserved.

